Antibiotics for community-acquired pneumonia: Is azithromycin out?
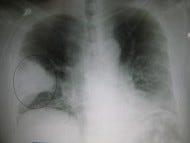
Is it time for a change in the standard treatment of community-acquired pneumonia? A new Dutch study says, maybe. The Infectious Diseases Society of America (IDSA) says, not so fast. IDSA's guidelines for treatment of community acquired pneumonia were last updated in 2007. For patients admitted to the hospital but not needing the ICU, they have advised either:
A "respiratory fluoroquinolone" (levofloxacin, moxifloxacin, or gemifloxacin), covering both typical (S. pneumonia) and atypical pathogens (Legionella, Mycoplasma, etc) OR
A ß-lactam (penicillin derivative or cephalosporin) plus a macrolide (azithromycin, clarithromycin or erythromycin) to cover atypical pathogens.
Times have changed since 2007. Fluoroquinolones got a black box warning from the FDA in 2008 for the risk of tendonitis and tendon rupture, with increased risk in patients older than 60. (Seizures, hallucinations, depression, QTc prolongation and torsade de points, and C. difficile colitis were also mentioned as rare adverse effects.) FDA issued a less dire "safety communication" in 2013 about azithromycin's potential for precipitating cardiac arrhythmias and sudden cardiac death. And in a study forming the basis for this warning, levofloxacin was associated with a similar risk of cardiovascular death as azithromycin. Why use these fluoroquinolones or macrolides at all? The benefits of fluoroquinolones or azithromycin over monotherapy with ß-lactams are argued to be 1) the coverage for atypical organisms, including the often-lethal Legionella, and 2) covering resistant strains of S. pneumonia. But (others say) atypical organisms cause a small minority of pneumonia cases, and exuberant prescription of azithromycin and fluoroquinolones could actually increase resistance to these drugs in the community. If narrower, safer antibiotic regimens could be used as standard therapy, better outcomes might result overall. The Netherlands-based CAP-START study just published in the New England Journal of Medicine tried to address this dilemma. In 7 Dutch hospitals, patients admitted to medical (non-ICU) wards with community-acquired pneumonia were randomly treated with either:
Beta-lactam alone (e.g. ceftriaxone),
beta-lactam plus macrolide (e.g. ceftriaxone and azithromycin), or
fluoroquinolone alone (e.g. levofloxacin)
To minimize the effect of hospital-based factors on study outcome, hospitals crossed-over to one of the other treatments every 4 months until full enrollment was achieved (2,283 patients). The trial was designed to test non-inferiority of beta-lactam monotherapy compared to the other 2 strategies. After 90 days, beta-lactam therapy mortality (9%) was non-inferior to that of beta-lactam/macrolide combination therapy (11%) or fluoroquinolone monotherapy (9%). Patients stayed in the hospital a median 6 days in all strategies, despite starting oral therapy a day earlier (3 vs 4) in the fluoroquinolone arm. The study wasn't designed to test antibiotic resistance, which occurs on a population level over years. Nor was it powered or designed to test the relatively rare incidence of severe adverse events (cardiovascular death, tendon rupture, anaphylaxis, etc) from any included drug.
What It Means
Should CAP-START change our standard approach to community acquired pneumonia treatment in the U.S.? PulmCCM interviewed Dr. Tom File, spokesperson for the Infectious Diseases Society of America (IDSA) to help us understand CAP-START. PulmCCM: Reading the results of CAP-START in the light of safety concerns with fluoroquinolones or azithromycin, can we now conclude that monotherapy with beta-lactams is adequate therapy for community-acquired pneumonia (CAP)? Dr. File: The short answer is no. I certainly applaud the authors for their study, but the findings do not change my position for the U.S. at this time. PulmCCM: Why not? Dr. File: Four reasons:
They designed the study for non-ICU patients and for those unlikely to have Legionella -- the two situations in which there is evidence of benefit of combination therapy that includes a macrolide (i.e., severe CAP and Legionella).
Second, there was very low identification of atypical pathogens in their study (e.g. Mycoplasma 0.4-1.8%) and their diagnostic methods were unclear to me. In most other studies of hospitalized patients there has been identification of atypical pathogens in greater than 10% of patients.
The use of 90-day mortality as an endpoint could obscure the benefits of combination therapy for atypical pathogens. Many non-Legionella atypical infections will eventually clinically resolve without effective antimicrobial therapy, but may take longer to do so. Thus, the primary outcome time point at 90 days in this study may be insensitive to differentiate a treatment effect between regimens.
Fourth, in the Netherlands study there was allowance for deviation from the initial antibiotic selection so as not to compromise care. It's worth noting there was more change from the beta-lactam arm (21.6%) than from the combination arm (15.2%) or the fluoroquinolone arm (12.5%).
PulmCCM: The IDSA community-acquired pneumonia guidelines were published in 2007. There has been a lot of new research, new drugs, as well as safety warnings since then. Is it time for an update to the IDSA guidelines? Dr. File: I agree a revision of the IDSA/ATS guideline is warranted to address several newer issues that have developed, including newer antimicrobial agents, use of immunomodifiers such as steroids, use of newer molecular tests to potentially provide earlier identification of etiology, as well as addressing some of the potential adverse effects of present antimicrobial agents, and to objectively assess all the newer studies regarding CAP. PulmCCM: What else do you see on the horizon that could change our approach to community-acquired pneumonia? Dr. File: As newer diagnostic tests become available, they may be able to provide a rapid diagnosis of the etiology of CAP even at the initial point of care so we potentially could provide pathogen-directed therapy right away, instead of using empiric therapy. If we knew the pathogen(s) at the point of care, we could potentially avoid use of overly broad-spectrum empirical therapy and instead give more targeted treatment -- reducing selection for resistance, potentially with lower cost and adverse effects (such as C. difficile infection). PulmCCM: Dr. File, thank you for your time and your insights. Read more: Antibiotic Treatment Strategies for Community-Acquired Pneumonia in Adults. N Engl J Med 2015; 372:1312-1323
β-Lactam Monotherapy vs β-Lactam–Macrolide Combination Treatment in Moderately Severe Community-Acquired Pneumonia: A Randomized Noninferiority Trial. JAMA Intern Med. 2014;174(12):1894-1901
Infectious Diseases Society of America/American Thoracic Society Consensus Guidelines on the Management of Community-Acquired Pneumonia in Adults. Clinical Infectious Diseases 2007; 44:S27–72.


