Overdiagnosis of pulmonary embolism on CT-angiogram by radiologists may be widespread
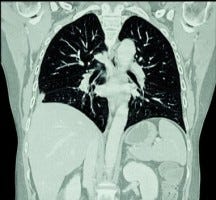
Contrasted CT-angiography of the chest, often called a "PE protocol CT," has dramatically improved the diagnosis of pulmonary embolism. When used in conjunction with validated clinical decision tools like modified Wells criteria, CT-angiography is highly sensitive (good at detecting PE when it's there and ruling it out when it's not) and specific (generating few false-positive results).
However, most CT-angiograms are ordered from emergency departments, often (usually?) without the use of clinical decision tools. When patients with low pretest probability are tested indiscriminately with CT-angiography, the false positive rate shoots up, as high as 40%.
Who gets to say what's a false positive pulmonary embolism on CT-angiogram? A subspecialized chest radiologist's opinion is considered the gold standard. If she disagrees with a general radiologist colleague's diagnosis of PE after reviewing the same images, overdiagnosis or a false-positive is considered to have occurred.
However, most CT-angiograms are interpreted by general radiologists without subsequent review by a chest radiologist. Almost no studies have sought to discover the actual false-positive or overdiagnosis rate for pulmonary embolism on chest angiogram when read by general radiologists. So what's the real world false positive rate among community radiologists reading CT-angiograms for pulmonary embolism?
A new single-center study testing just that question found that more than a quarter of diagnosed pulmonary emboli were false-positives, including almost half of solitary PEs and more than half of subsegmental PEs. Barry Hutchinson et al publish their findings in the American Journal of Roentgenology.
Authors reviewed almost 1,000 CT-angiograms performed over 1 year at a university hospital in Ireland, of which 174 were initially read as positive. A panel of three chest radiologists then reviewed the 174 positive scans, only reversing the initial diagnosis if all 3 agreed there was no PE. This resulted in an observed false-positive rate of 26% overall; 46% among solitary PEs, 27% among segmental PEs and 59% among subsegmental PEs.
If these findings reflect even partial reality in the U.S., thousands of people are being prescribed long-term anticoagulation unnecessarily every year. For pulmonary emboli that are considered unprovoked, current guidelines advise consideration of "indefinite" anticoagulation -- which is a long time if you didn't ever have a blood clot in the first place.
One shouldn't overreact to a single center study on another continent, and we should also mind the potential psychological biases here: these radiologists knew they were reviewing old scans, and that they were not at risk for failing to make a PE diagnosis. This could have made them less conservative in interpreting than a real-world radiologist. Because they were allowed to talk and interact to come to consensus, other human factors could come into play. A complementary but more difficult study would compare non-specialized radiologists to chest radiologists prospectively reading CT-angiograms, and compare their interobserver variability.
Nonetheless, this study adds to a major database analysis published in 2011, which strongly suggested that in the United States, pulmonary embolism is being overdiagnosed (and thus over-treated with anticoagulation) since the introduction of CT-angiography around 1998.
That study suggested complications of anticoagulation for pulmonary embolism may be rising substantially in association with excess CT-angiography, as well.
There is a recent trend in research testing the use of age-adjusted d-dimers (which rise with age in otherwise healthy adults) as components of modified decision making tools to avoid the unnecessary use of CT-angiogram altogether. No test = no possibility of a false positive, no unnecessary anticoagulation, no excess bleeding.
Clinical Takeaway: Clinical decision tools deployed in the emergency department can improve the accuracy and value of CT-angiography in the evaluation of dyspnea; not using them will result in avoidable false positive pulmonary embolism diagnoses. Consider getting a second opinion from a chest radiologist on CT-angiograms read initially as positive for solitary pulmonary embolism, or at the segmental or subsegmental levels.
Read more:
Hutchinson BD et al. Overdiagnosis of Pulmonary Embolism by Pulmonary CT Angiography. AJR Am J Roentgenol. 2015 Aug;205(2):271-7. doi: 10.2214/AJR.14.13938.


