Pirfenidone prolongs survival, preserves lung function in idiopathic pulmonary fibrosis (ASCEND)
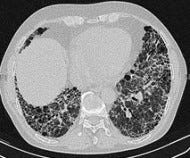
For idiopathic pulmonary fibrosis treatment pirfenidone, the third time wasn't the charm; the fourth was.
After reducing decline in forced vital capacity over one year in a Japanese trial of 275 IPF patients, pirfenidone went one-and-one in the multinational CAPACITY trials (n=779), meeting the primary outcome of FVC preservation in one but not the other. The U.S. FDA asked for a tiebreaker, and the ASCEND trial was born. Several years and many millions of InterMune dollars later, ladies and gentlemen, we have an answer:
Pirfenidone reduced the decline of lung function, improved progression-free survival and prevented loss of exercise tolerance in people with idiopathic pulmonary fibrosis, as compared with placebo.
Talmadge King et al reported the ASCEND trial results at the American Thoracic Society annual meeting and in the May 18 2014 New England Journal of Medicine.
ASCEND enrolled 555 patients from 127 sites in 9 countries, mostly in the U.S. Subjects had clinical-radiographic or biopsy-confirmed IPF, and mild to moderate restrictive lung disease (forced vital capacity 50-90% predicted) along with diffusion impairment on pulmonary function testing. The CAPACITY enrollment criteria were tweaked for ASCEND to try to capture people at higher risk for disease progression (e.g., excluding those with comorbid COPD, and including more with worse diffusion impairments). They were randomized 1:1 to pirfenidone or placebo and followed for one year.
After 52 weeks, only half as many patients receiving pirfenidone had a significant decline in FVC (≥10% predicted) as did placebo patients (46 vs. 88 respectively). More than twice as many subjects taking pirfenidone lost no lung function (63 vs. 27), and slightly fewer patients taking pirfenidone had a decline in 6 minute walk distance by ≥50 meters.
Pirfenidone did not reduce mortality compared to placebo in the ASCEND trial. However, when ASCEND's results were pooled with those from CAPACITY and the Japan trial, patients taking pirfenidone had half the risk of death from all causes, and one-third the risk of death from idiopathic pulmonary fibrosis (0.52 and 0.32 hazard ratios respectively, compared to placebo). The pooled numbers (n=1,247) showed:
22 deaths of any cause on pirfenidone, vs. 42 on placebo
7 deaths attributable to IPF (pirfenidone) vs. 22 (placebo)
By my math, that's an impressive number needed to treat of 63 with pirfenidone for one year to prevent one death (can someone please double-check this). There were no serious safety signals and few adverse events: anorexia, vomiting, stomach pain, reflux were significantly more common in the pirfenidone group, infrequently leading to drug discontinuation.
The exciting results for pirfenidone in ASCEND and nindetanib in INPULSIS could herald a new era of treatment for IPF, an illness that had seemed impervious to treatment despite decades of biomedical research and innovation. Finally, something that works!
But I'm starting to sound like a press release. I hope I wasn't influenced by InterMune's ghostwriting team, who wrote the first draft of the New England paper. Can't Talmadge King of all people be allowed to write his own manuscripts? Sadly, no -- not when billions of dollars and a biotech company's future are at stake. (InterMune's stock price fell from a high of $51 to $11 when FDA declined approval in 2010. It's back up around $40 at this writing.)
Pirfenidone has been available internationally as Esbriet for several years. With ASCEND, FDA approval in the U.S. seems imminent, and pirfenidone will soon become the first proven effective treatment for idiopathic pulmonary fibrosis (or the second, depending on its competitor nindetanib's status). That news may be literally lifesaving for the thousands of people living with IPF whose disease is destined to progress. And doctors can finally feel like doctors rather than feeling helpless and pathetic in the face of this humbling disease.
Of course, it's also great for InterMune, because contrary to accepted wisdom about the natural course of idiopathic pulmonary fibrosis, a majority of people with the diagnosis experience very slow (or absent) progression of disease (which may be why it's been so hard to prove pirfenidone's benefit). That means they could be taking pirfenidone and generating revenue for years, during a disease course that would have been long and stable anyway. InterMune's next challenge will be to price the drug: expect it to be just high enough to provoke outrage among payers, but not so high as to drive policymakers to impose restrictions on physicians' open prescription of pirfenidone for anyone with IPF, of any severity. To that end, watch out also for big-time "awareness campaigns" in direct-to-consumer advertising, most likely through surrogate nonprofit disease advocacy organizations, to try to bring these nonprogressing IPF patients and their doctors into lifelong pirfenidone prescriptions.
Talmadge King et al. A Phase 3 Trial of Pirfenidone in Patients with Idiopathic Pulmonary Fibrosis. NEJM May 18, 2014. DOI: 10.1056/NEJMoa1402582.


