Polymyxin B "blood purification" for sepsis is in trouble
FDA isn’t biting on TIGRIS data ... yet
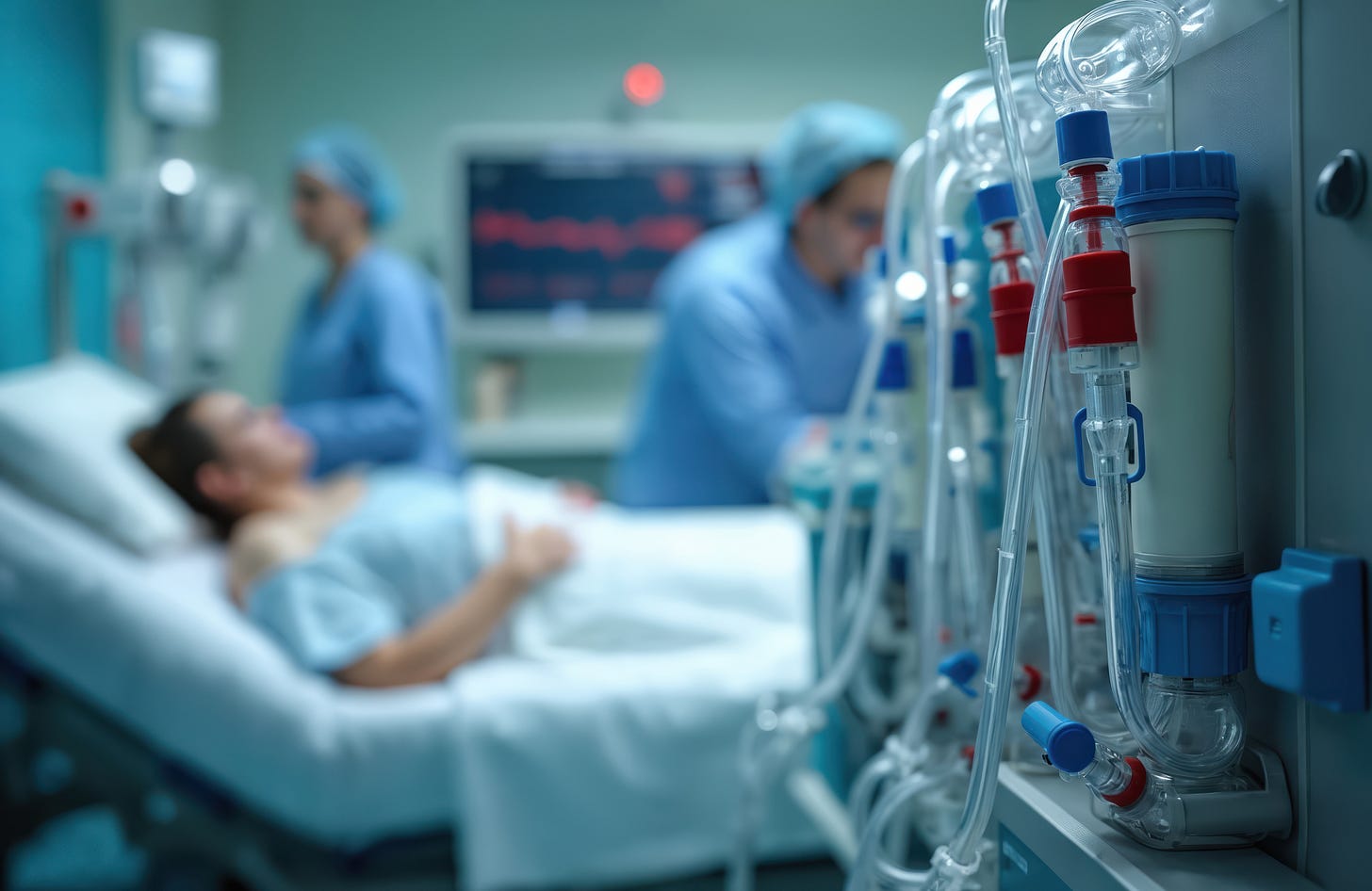
Hemoperfusion and hemadsorption are so-called “blood purification” technologies that can remove endotoxin, cytokines, or other potentially deleterious proteins from the bloodstream in sepsis or other medical conditions.
These are extracorporeal circuits (often running on CRRT machines) that pump blood through a matrix that attracts or adsorbs the offending proteins in bulk before returning the “purified” blood to the patient.
FDA set to approve "blood purification" for sepsis?
Sepsis is sometimes called “blood poisoning” by laypeople, and they’re not wrong. Can the blood of patients with sepsis be removed from their bodies, detoxified, and returned, saving lives in the process?
Blood purification technologies have regulatory approval in multiple countries in Europe, Asia, Canada, and elsewhere, but not yet in the U.S.
That’s primarily because although they do remove the proteins they are designed to, blood purification has never been demonstrated to improve outcomes in sepsis.
Spectral Medical, makers of an endotoxin-removal device using polymyxin B and marketed as Toraymyxin™, would like you to believe otherwise.
The TIGRIS trial’s results were published in Lancet Respiratory Medicine in March 2026.
It concluded that among a selected group of sepsis patients with endotoxin levels in a “Goldilocks” zone (not so low or high that removal wouldn’t help), the likelihood that polymyxin B hemoperfusion saved lives was >99%.
However, the path to this conclusion was more winding (and fanciful?) than any fairytale, relying on p-hacking, aggregating pools of patients across clinical trials, and Bayesian probabilities rather than standard (“frequentist”) statistical calculations.
In other words, “precision medicine.”
It went down like this:
The EUPHAS (2009) trial was stopped early at n=64 when it seemed that polymyxin hemoperfusion (PMX) reduced mortality in sepsis.
But ABDOMIX (2015) suggested harm among patients undergoing emergency surgery for peritonitis.
EUPHRATES (2018) then became the lodestar of hemoperfusion. The trial did not show a mortality benefit from PMX over sham treatment in a multicenter, randomized trial of 450 patients with severe sepsis and high endotoxin activity (EAA level ≥0.60) at 55 tertiary hospitals in North America, from 2010 to 2017.
Nor was there a benefit in the sickest patients with high organ failure scores. Nor did patients treated with hemadsorption in EUPHRATES experience a reduction in endotoxin activity compared to sham-treated patients.
However, post-hoc analysis found that the 194 patients in EUPHRATES with endotoxin activity levels between 0.60 and 0.89 had a non-significant reduction in 28-day mortality with polymyxin hemoperfusion (26% vs 37%, p=0.11, reduced to 0.047 after adjustment).
This endotoxin zone of 0.60 to 0.89 units was then used as the “precision” in the future “precision medicine” TIGRIS trial design.
TIGRIS Trial: Can I Borrow a Cup of Patients?
TIGRIS enrolled 194 septic patients, or 1% out of an enormous ~15,000 screened. They were all very sick and had endotoxin activity levels between 0.60 and 0.89. They were randomly assigned 2:1 to receive PMX hemoperfusion or usual care (treatment assignment was not blinded).
The “real” (legible, familiar, frequentist) results were:
No mortality difference at 14 days (34% PMX vs 37% control)
90-day mortality: A trend toward benefit with PMX (HR 0.68 [0.43 - 1.07]), with separation occurring around 28 days.
The authors also used an unusual technique of combining the TIGRIS patients with the (post-hoc fished-out) EUPHRATES cohort. This is called “historical borrowing,” but it is not simply pooling the patients and then performing traditional statistical analysis on the dataset. Rather, the earlier patients are used as weighting factors in a complicated Bayesian modeling scheme. This weighted Bayesian analysis produced the reported 99% likelihood of an improvement in 90-day survival with PMX.
Guidelines came out before TIGRIS
The Surviving Sepsis Campaign (PulmCCM has no affiliation) in its latest guideline update, gave polymyxin B hemoperfusion (along with related technologies) one of its rare raspberries: a thumbs-down for patients with sepsis:
We ‘suggest against’ using blood purification techniques, including hemoperfusion, high-dose hemofiltration, or plasma exchange. … we ‘suggest against’ using polymyxin B hemoperfusion.
They noted the evidence was weak either way and this was a conditional (weak) suggestion (like nearly all of the other recommendations).
However, the committee did not have full access to the published TIGRIS data— although preliminary data was available prior to the guidelines publication.
New Sepsis Guidelines Released!
Sepsis has an ontological problem—after hundreds of years, we still can’t coherently say what it is, and clinical intuition remains the primary criterion for its diagnosis.
The “Theranostics” Business Model
It’s likely that even if a benefit were confirmed, only a fraction of patients with sepsis would be eligible for treatment with PMX hemoperfusion (note the 1% enrollment rate from ~15,000 screened).
But Spectral Medical also licenses/sells the endotoxin activity assay that would serve as a screening test for PMX hemoperfusion eligibility. FDA approval of Toraymyxin™ could allow Spectral Medical to market the endotoxin assay as an appropriate test for a large proportion of patients presenting with severe sepsis.
Controlling both the treatment and the test for its eligibility in this way is dubbed “theranostics” on the business side (i.e., diagnostics + therapeutics, but “diagpeutics” didn’t roll off the tongue as well).
Spectral Medical has estimated the total annual U.S. market for PMX hemoperfusion plus its endotoxin assay at about $1.5 billion. A possible price for the PMX cartridge was ~$7,500 in an investor presentation, with about $300 million in annual revenue for both PMX + EAA with strong market penetration. (The endotoxin test was only expected to bring in ~$10 million per year.)
The company’s financials suggest a small startup dependent on investor capital and debt: they reported having about $1.5 million in cash and ~$9 million in debt in March 2024, with only about $1.6 million in annual revenue (USD).
Baxter controls about half the U.S. market for CRRT machines, which would allow for efficiencies in the marketing and distribution of PMX cartridges.
FDA Unconvinced So Far
Toraymyxin™ received a breakthrough medical device designation from the FDA in 2022. Spectral Medical and its major investor, Vantive (a spinoff from Baxter), reported that the FDA had agreed to their Bayesian analysis of the combined EUPHRATES and TIGRIS data rather than a larger conventional trial. The company previously announced it would seek full FDA approval as soon as Q1 2026.
However, their subsequent press releases suggest that FDA has requested additional data (e.g., on longer-term survival in TIGRIS). FDA approval will not occur until January 2027 at the earliest, the company has signaled to investors.
There do not seem to be any randomized trials in process or planned testing polymyxin hemoperfusion for sepsis, and the endotoxin/polymyxin theranostics platform is Spectral Medical’s major offering outside its small reagents business. It seems likely that the firm will live or die by the FDA’s approval decision.
Imprecise Enthusiasm
In any industry-funded randomized trial with n<200, a non-significant trend toward a mortality benefit in an experimental therapy should prompt skepticism, and TIGRIS is no exception.
But they put in the work. The TIGRIS trial was a successful execution of a very difficult trial design, and an achievement worth recognizing.
Its use case may be extremely narrow. It might not, in fact, improve outcomes at all. Hundreds of millions or billions of dollars may be spent on endotoxin tests and PMX cartridges only to enrich Vantive’s and Spectral’s stockholders, before the therapy is finally disproven.
Ten years ago, that would have prompted reflexive scorn in this newsletter.
But the limited data for 90-day mortality in TIGRIS suggest there’s a chance that it might help. And in the sprawling junkyard of failed treatments for sepsis, the plausible hope that something might eventually be shown to work is still worth rooting for. With less than 99% enthusiasm, to be sure—but some.
The question is whether that hope justifies launching what would be in effect a taxpayer- and insurer-funded, population-level postmarketing observational study on patients with endotoxin-predominant sepsis.
Does it?
Reference
Neyra JA, Legrand M, Tidswell MA, et al. Polymyxin B haemoadsorption in endotoxic septic shock (Tigris): a multicentre, open-label, Bayesian, randomised, controlled, phase 3 trial. The Lancet Respiratory Medicine. Published online March 2026. doi:https://doi.org/10.1016/s2213-2600(26)00047-0




One minor correction. SSC guidelines are based on published literature, and the data analysis for our recent publication were locked nearly a year before the publication of TIGRIS. The guidelines were released one or two days before TIGRIS results were, both at the recent SCCM Congress. I won't hazard a guess at how the guideline committee would have dealt with these data, but "ample access" to the data is off the mark.
Excellent points dubious effect for sure - why does Europe allow? Thought we and our system of too much spending for worse results at least had the “benefit” of a safe haven for medical innovation - pt harm be less of a concern.