What works to help people with pulmonary fibrosis feel better? (Review)
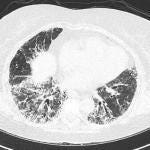
Interventions to Improve Symptoms, Quality of Life in Fibrotic ILD: Do They Work?
Patients with fibrotic interstitial lung diseases (e.g. idiopathic pulmonary fibrosis) have a poor overall prognosis, and there are no therapies proven to halt disease progression or extend life. Further, many of these patients have debilitating symptoms, limited functional capacity, and poor quality of life. So absent effective disease modifying treatments, wouldn’t it be nice to at least help these patients feel and function better? Such interventions are the focus of a recent systematic review and meta-analysis performed by Sabrina Bajwah et al, reported in Thorax.
What They Did
The authors performed a thorough literature search for interventions in fibrotic interstitial lung diseases that report outcomes for symptoms, functional capacity (measured by 6-minute walk distance), and quality of life. They included randomized controlled trials (RCT), non-randomized trials, and observational studies. They also performed meta-analyses for interventions that had more than one RCT. The strength of evidence was ranked as “strong” (supported by meta-analysis of more than one RCT), “moderate” (supported by one RCT), and “weak” (supported by non-RCT studies).
What They Found
They included 34 papers (35 total studies) with a total of 3,535 patients (3,419 had IPF). Instruments for measuring symptoms and quality of life varied widely among studies making comparisons difficult. Interventions reviewed included interferon gamma-1b, sildenafil, bosentan, pirfenidone, n-acetylcysteine, co-trimoxazole, etanercept, iloprost, D-pencillamine, interferon alpha, ribavirin, colchicine, doxycycline, prednisolone, pulmonary rehabilitation, disease management programs, supplemental oxygen, diamorphine, and thalidomide. Tables 2 and 3 in the paper provide an excellent evidence summary for those interested in more details for each intervention. Here are the major findings:
Functional capacity: pulmonary rehabilitation (strong evidence), pirfenidone (strong evidence), and supplemental oxygen (weak evidence) all improved six-minute walk test distance.
Quality of Life: pulmonary rehabilitation and sildenafil improved or preserved some quality of life measures (both with moderate evidence); thalidomide and doxycycline had weak evidence.
Symptoms:
Dyspnea: prednisolone (but remember, steroids plus azathioprine increase mortality in IPF), diamorphine, D-pencillamine, and colchicine all had weak evidence; pulmonary rehabilitation had a mixed effect; sildenafil preserved dyspnea compared to placebo in the largest trial as measured by the UCSD SoBQ but not by the Borg score, which was the metric used to combine data with a much smaller trial for their meta-analysis, so not surprisingly their meta-analysis was negative for an impact of sildenafil on dyspnea
Cough: interferon alpha and thalidomide (weak evidence)
Anxiety: diamorphine (weak evidence)
Fatigue: pulmonary rehabilitation (weak evidence)
What It Means
Arrgh! As I suspected, we don’t have much to offer patients with fibrotic ILD in the way of symptom relief. Clearly a lot of work needs to be done to figure out how to palliate these patients, probably starting with standardizing meaningful outcomes for symptoms and quality of life to allow for better comparisons among therapies. Here’s my take-away from the available evidence:
Supplemental oxygen (with optimal titration during exertion) and pulmonary rehabilitation seem like no brainers considering their potential benefits and few downsides (e.g. cost and inconvenience).
Sildenafil might be worth a try for preservation of quality-of-life (and possibly dyspnea) in those with advanced disease (i.e. DLCO < 35% predicted).
Opiates may be used for selected patients, especially for those nearing the end of life, to relieve dyspnea and anxiety.
Thalidomide looks promising for treating cough (an often debilitating symptom in IPF) in this trial (published after the lit search for this paper) but needs further study.
While the jury is still out on the benefits of pirfenidone for impacting disease progression and mortality (we eagerly await the results of the ASCEND trial), it seems like quite an expensive (and not yet FDA-approved) therapy if used only for helping people walk a little bit further.
The other interventions listed here are clearly not useful, have insufficient evidence, or have risks that outweigh potential benefits. Sabrina Bajwah et al. Interventions to improve symptoms and quality of life of patients with fibrotic interstitial lung disease: a systematic review of the literature. Thorax 2012: online first.


