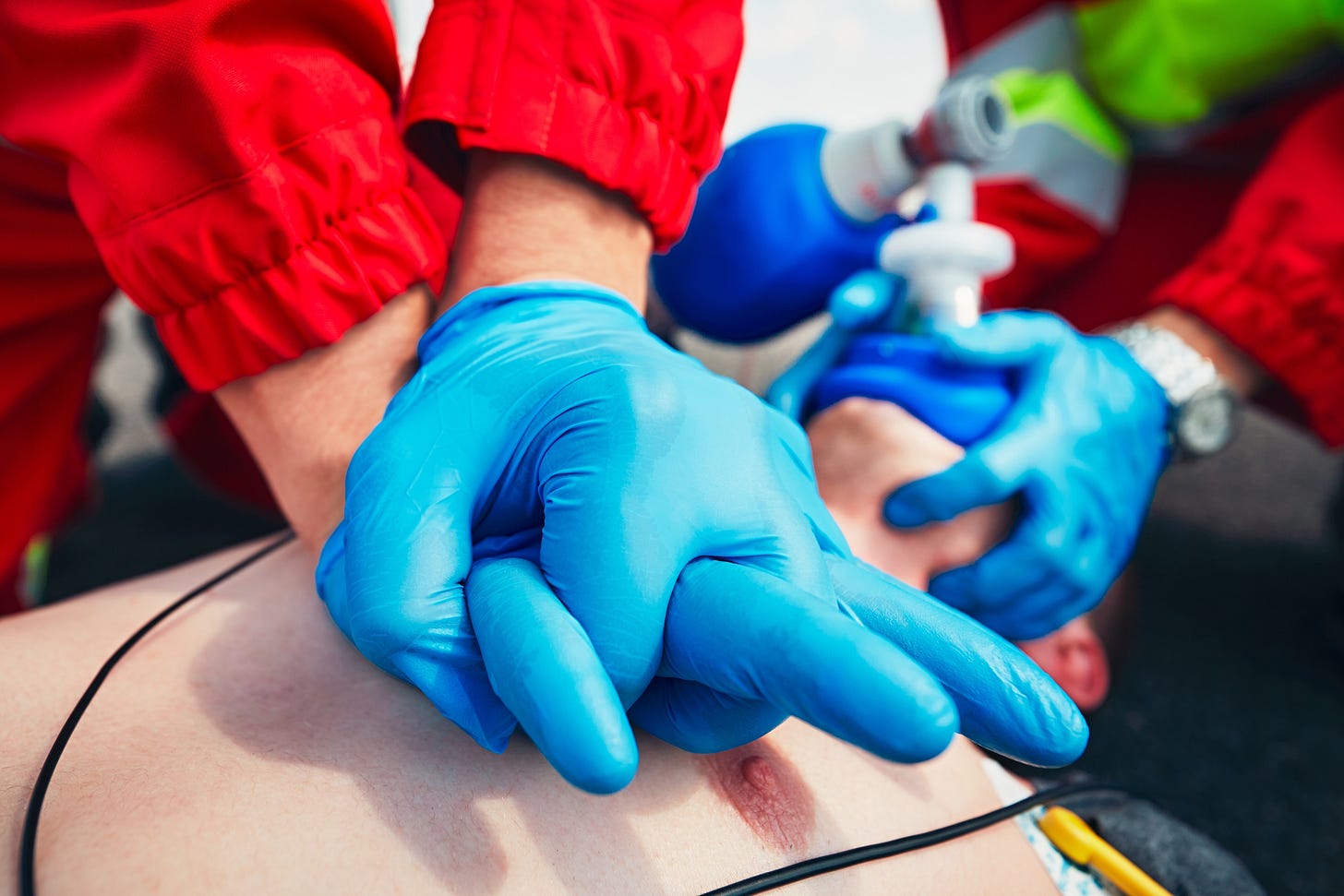
Temperature control after cardiac arrest does not improve outcomes ... right?
Hope stays alive to keep cooling cool
Is it too easy to say it was all a fever dream?
There was good reason to be optimistic in 2002 that induced hypothermia would improve survival and neurologic outcome after cardiac arrest. Animal studies aligned with anecdotal evidence from victims of drowning in frigid waters: colder temperatures preserved brain. Two “landmark” trials on out-of-hospital cardiac arrest seemed to confirm the preclinical data. Practice changed quickly; guidelines enshrined the practice of cooling all cardiac arrest patients.
Twenty-four years and 11 large randomized trials later (all negative except the equivocal HYPERION), guideline authors walked back from “cool them all” to “prevent all fevers” by actively maintaining normothermia (≤37.5°C) with external cooling systems like Arctic Sun™.
Those guidelines, however, still tacitly encouraged hypothermia by specifying a range of 32° to 37.5°C as appropriate temperature targets.
The awkward truth was that maintenance of normothermia was not itself known to be beneficial, because it had never been tested. After the original trials favoring hypothermia (likely spuriously, in hindsight), allowing fevers was presumed to be unethical.
The supposed benefits of fever prevention were inferential, based on highly confounded observational studies correlating fevers with worse outcomes in strokes. The obvious problem: larger strokes cause both fevers and bad outcomes.
Randomized trials testing fever prevention in strokes (most notably the INTREPID trial, Greer et al JAMA 2024), showed no benefit of the practice.
It might be too embarrassing and heterodox for academics to run a large randomized trial that could establish that doing little or nothing temperature-wise is the best approach.
Thus, we will likely only have the findings of observational studies to consider.
Temperature Management for In-Hospital Cardiac Arrest
The most recent data for IHCA comes from the “Discover In-Hospital Cardiac Arrest” cohort (Andrea et al Crit Care Med 2026).
In 2023-2024, a major U.S. critical society guided 46 participating hospitals in multiple nations in a prospective observational cohort study assessing the use of targeted temperature management and outcomes among 1,006 patients achieving ROSC after in-hospital cardiac arrest, among whom 615 remained alive and comatose and eligible for TTM.
Adherence with TTM was generally low, and had no observed association with mortality or improved neurologic status at discharge.
In more than half, the treating teams did not document any strategy to manage temperature.
30% of patients had targeted normothermia (≤37.5°C) or fever avoidance as their strategy.
In 14% (85 patients), hypothermia was targeted, usually 36°C.
There was only one consistent outcome resulting from fever prevention: fewer fevers.
“Patients with documented strategies received more temperature management therapies and had a lower burden of fevers, but there was no association with outcomes.”
But Many Single-Center Observational Studies Suggest Benefits of TTM …
Yet it’s easy to find multiple retrospective observational series that found an association between hypothermic temperature management (e.g. 33°C) and improved outcomes after out-of-hospital and in-hospital cardiac arrest.
One of the most prominent and recent was a single-center retrospective study at U. of Pittsburgh (Callaway et al JAMA Ntwk Open 2020).
Among 1,319 patients admitted to one center after out-of-hospital cardiac arrest, cooling to 33°C was associated with better survival and neurologic outcomes compared to TTM at 36°C, in more severely ill patients (shock and/or deeper comas).
However, in the less severely ill, 36°C was associated with improved outcomes.
The magnitudes of effects were large in both subgroups—in opposite directions: 14% “harm” of 33°C in the less-ill vs 22% “benefit” of 33°C in the sicker patients. Almost two-thirds of patients died after withdrawal of life support.
In the context of negligible or no benefit of TTM in multiple randomized trials, this data pattern strongly suggests clinician bias in selecting which patients were targeted at which temperatures. Authors noted that (based on their interviews with clinicians),
Treating physicians were more likely to select TTM at 36°C for patients they believed had nonsurvivable illness or with antecedent goals of care that limited critical care support … Assignment of a few more moribund patients to TTM at 36°C would bias our results to favor TTM at 33 °C.
The higher proportion of deaths in TTM at 36°C vs TTM at 33°C attributed to multiple organ failure (39.5% vs 27.3%) or WLST for nonneurologic reasons (25.3% vs 11.0%) suggests that this bias is present.
The transparency of this discussion is laudable. The Pitt data highlights the limitations of retrospective observational data from any single institution when clinician discretion has an overarching influence on the final outcomes.
… While Larger Registries Tell a Different Story
The most robust and compelling data regarding temperature management after in-hospital cardiac arrest come from a large retrospective observational cohort derived from the AHA’s Get With the Guidelines registry.
The outcomes for over 26,000 patients at 355 U.S. hospitals who achieved ROSC after an in-hospital cardiac arrest between 2002 and 2014, who were either treated hypothermia or not were analyzed.
One interesting finding is just how few hospitals were cooling IHCA patients during this time: only 1,568 (6%) were treated with hypothermia, although most were comatose.
Patients treated with hypothermia were more likely to die in the hospital or to have a poor neurologic outcome (about a 2% absolute difference for either), compared to propensity-matched patients not treated with hypothermia.
Bias was certainly also present in these decisions, but the direction and magnitude of the finding observed across many more systems is more informative than any single-center cohort.
Why Prevent Fevers After Cardiac Arrest?
Guidelines still advise temperature management to prevent the supposedly harmful fevers after cardiac arrest.
With the benefit of hindsight, this should have been the first intervention to test, not the last—i.e., active maintenance of normothermia vs. usual, reactive care only.
After the massive efforts poured in, the guidelines written and unwritten, a total lack of benefit here might be too much to accept, though. “Temperature management” still provides us with something to do in a usually terrible situation that might be helpful.
Accordingly, no randomized trials are underway with a control arm allowing for a “pre-2002 usual care” response to fevers (e.g., acetaminophen only).
The hope for a benefit from hypothermia is still alive, albeit on life support. The SAVE-J NEUROTHERM and the R-CAST OHCA studies are ongoing in Japan. The Europeans have PRINCESS2 approaching coronation (after the first PRINCESS was deposed). And in the U.S., although ICECAP quietly shut down in 2025 for futility, its pediatric version continues.
Hope is always good. Just don’t call hypothermia “therapeutic” anymore, please.
References
Andrea L, Berg KM, Johnson NJ, et al. Temperature Control After In-Hospital Cardiac Arrest: Outcomes From the Discover In-Hospital Cardiac Arrest Cohort. Critical Care Medicine. Published online March 20, 2026. doi:https://doi.org/10.1097/ccm.0000000000007121
Chan PS, Berg RA, Tang Y, Curtis LH, Spertus JA; American Heart Association’s Get With the Guidelines–Resuscitation Investigators. Association Between Therapeutic Hypothermia and Survival After In-Hospital Cardiac Arrest. JAMA. 2016 Oct 4;316(13):1375-1382. doi: 10.1001/jama.2016.14380. PMID: 27701659; PMCID: PMC5486217.
Callaway CW, Coppler PJ, Faro J, Puyana JS, Solanki P, Dezfulian C, Doshi AA, Elmer J, Frisch A, Guyette FX, Okubo M, Rittenberger JC, Weissman A. Association of Initial Illness Severity and Outcomes After Cardiac Arrest With Targeted Temperature Management at 36 °C or 33 °C. JAMA Netw Open. 2020 Jul 1;3(7):e208215. doi: 10.1001/jamanetworkopen.2020.8215. PMID: 32701158; PMCID: PMC7378753.