The Real-World Boards: Question #38
Seizure, hypertension, intubation. What now?
These are the Real-World Boards. As in the real world, there may be no single “right” answer, and you are only competing against yourself. Upgrade to the Lifelong Learner level for full access to all the questions and unlimited CME credits with an included Learner+ account.
A 51-year-old woman is brought to the ED after a witnessed seizure at home after she complained of headaches and then became confused. She had another generalized seizure in the ambulance and a third in the ED. She is intubated for status epilepticus and loaded with levetiracetam. Neurology are consulted.
According to her family, she was diagnosed with rheumatoid arthritis this year, for which she now takes a tumor necrosis factor-alpha antagonist, with good disease control. She also takes metoprolol for hypertension. She has never had a seizure before today.
Her blood pressure was initially 200/110 and is now 165/85 with a nicardipine infusion. Other vital signs and labs are unremarkable. She is sedated on propofol and poorly responsive.
A CT of her head showed no acute process. An EEG is ordered. High-dose ceftriaxone, acyclovir, and vancomycin are infused IV.
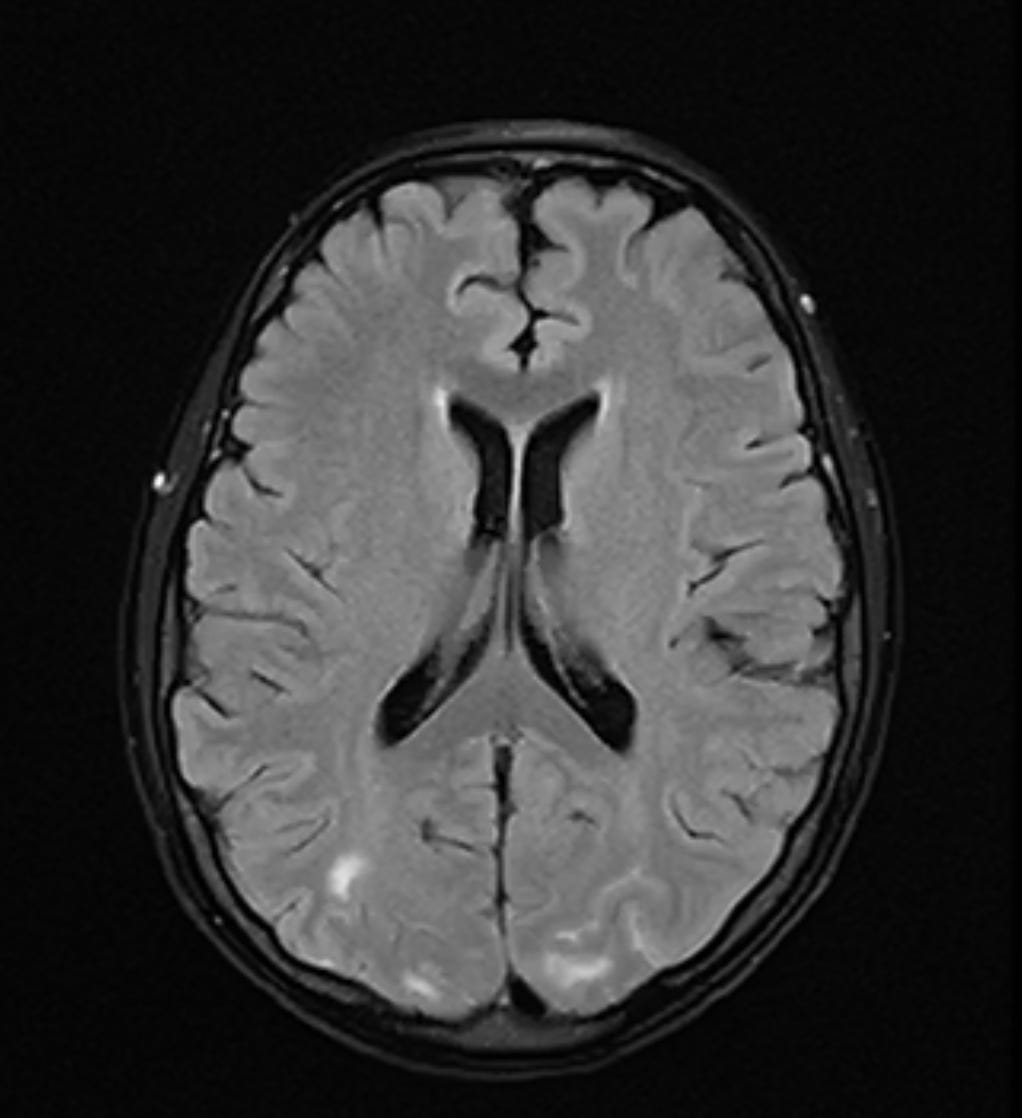
A stat brain MRI is obtained: